CBC’s Muddied Water: 1919 podcast explored a city divided by the conditions that led to the Winnipeg General Strike. In this bonus episode, we explore the flu pandemic that hit the city one year and similarities now 100 years later to the COVID-19 pandemic.
A few months ago, the only curves most people cared about involved their own waistlines. COVID-19 gave new meaning to the term.
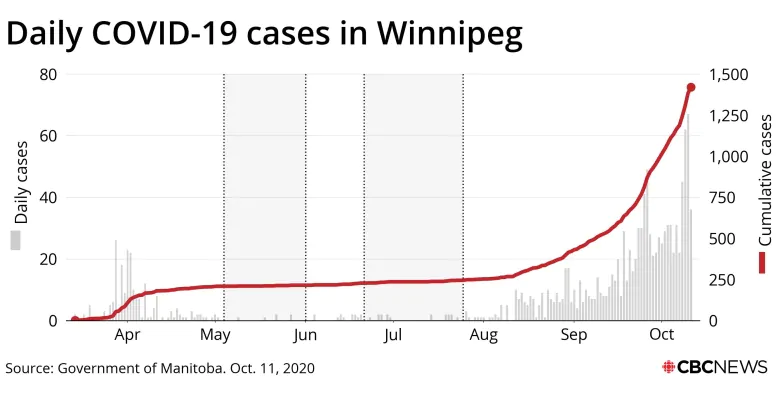
Since the coronavirus pandemic was declared in March, public health officials have urged citizens to “flatten the curve” — the figure in question being the bell-shaped curve of the now-familiar line chart that illustrates the daily number of people with active cases of the virus known as SARS-CoV-2.
The COVID-19 curve in Winnipeg rose slightly in late March and early April, flattened out almost entirely during the spring and summer and then jumped dramatically in September, when the number of cases spiked in Manitoba’s capital.
As much as Winnipeggers may not want to hear this, we can still only see the beginning of the COVID-19 curve. This pandemic will play out for many more months, if not several years.
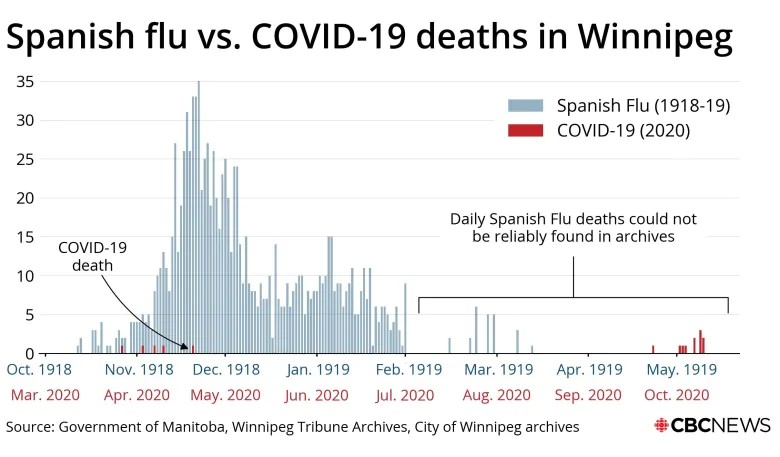
But we can already see how the initial ascent of the COVID-19 curve compares with the last pandemic curve in Winnipeg.
More than a century ago, what’s known as the Spanish influenza largely skipped Manitoba during its initial worldwide wave late in the winter of 1918.
The second wave of the pandemic, in the fall of 1918, hit Winnipeg hard, with a spike that quickly escalated out of control. There were several thousand infections in a matter of weeks.
The influenza curve did not flatten out in Winnipeg until thousands of residents contracted the disease.
The two curves bear little resemblance, partly because of the viruses themselves — but mostly because of the immense changes to modern medicine, public health, personal hygiene and the way people live.
Some of those changes were necessitated by the severity of the 1918-20 influenza pandemic.
Entirely different pandemic curves
Using newspaper and medical archives, it’s possible to piece together several months worth of daily case counts for the 1918-20 influenza pandemic and compare the infections to the course of COVID-19.
The first publicly reported case of Influenza in Winnipeg was on Oct. 1, 1918. “Spanish ‘Flu’ here,” the Manitoba Free Press proclaimed on Page 5.
By Oct. 12, authorities had already shut down schools and public gathering spaces, such as theatres and meeting halls.

The initial response to the Spanish flu has one parallel to the response to COVID-19. There were 11 days between the first reported infection and the closure of schools in both 1918 and 2020.
University of Manitoba history Prof. Esyllt Jones is not surprised by the authorities’ rapid move to shut things down 102 years ago.
“Daily experience with infectious disease was more frequent then than it is now,” said Jones, the author of Influenza 1918: Disease, Death, and Struggle in Winnipeg.
Diseases such as diphtheria, measles, mumps, whooping cough and tuberculosis were still common.
“So most public health people of that generation were really quite experienced dealing with issues of transmission,” Jones said.

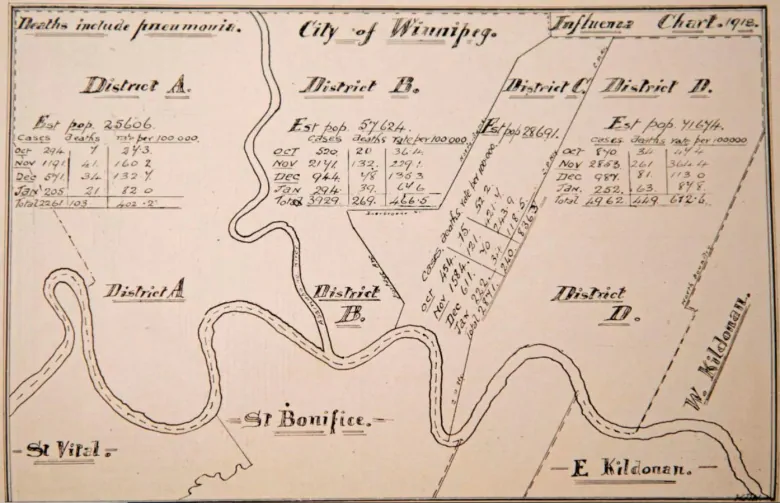
Despite the early imposition of physical distancing measures in the fall of 1918, the Spanish flu ripped through Winnipeg, home to just under 180,000 people at the time. By Jan. 1, 1919, 12,950 people in Winnipeg were infected.
Crowded housing was a significant factor in the rapid spread, Jones said.
“It’s a respiratory disease. It’s winter. People are living in crowded living conditions, and when someone gets infected, there’s really no way to isolate that person,” she said.
City of Winnipeg assessment data says homes built prior to 1920 that remain standing have an average living space of just over 1,200 square feet.
These homes would have housed on average of 4.6 people under each roof when the influenza epidemic arrived, Statistics Canada says.
As of the last census, in 2016, the average Canadian household has almost half as many people.
A century ago, there was no scientific ability to test for the virus. Identifying asymptomatic carriers was impossible. This made quarantine guidelines and contact tracing an exercise in futility.
As well, there was no such thing as “remote work” 75 years before residential internet service became commonplace. After the end of the First World War, many homes still didn’t even have telephones.
A second Winnipeg spike of Spanish flu cases, during the spring of 1919, was much smaller relative to the initial local spike. The virus eventually petered out in the Manitoba capital during the summer of 1919.
This differs from COVID-19. The initial Winnipeg spike this spring, which was mostly the result of returning international travellers, has been dwarfed by a September wave caused mostly by close-contact and community transmission.
Antibiotics would have saved lives
As of Saturday, COVID-19 had claimed the lives of 16 Winnipeggers. In 1919, by the time the Spanish flu had largely run its course in Manitoba, the virus had killed more 1,200 people in the provincial capital.
Dr. Jason Kindrachuk, an associate professor and Canada research chair in emerging viruses at the University of Manitoba, said the higher death toll for the influenza epidemic is no surprise, given the state of medicine and public health a century ago.
“I say that without minimizing what we’re going through with [COVID-19],” said Kindrachuk, who has studied the 1918-20 pandemic and is engaged in COVID-19 research.
It’s hard to do a comparative analysis of the two pandemics because a number of factors have changed since 1918, he said.
“In 1918, if there was no underlying immunity, there was no vaccine. There were no therapeutics. Same case we’re in with [COVID-19], with the exception that [in 1918] we also didn’t have all the additional measures from a health-care standpoint that we have now,” he said.
During the Spanish flu epidemic, the vast majority of patients who died were killed by opportunistic bacterial infections that afflicted people whose bodies and immune systems were weakened by influenza, Kindrachuk said.
The death toll from the flu would have been reduced dramatically had antibiotics been available. They were not developed for another two decades.
Other medical practices also played a role. Ventilators that help people breathe were not yet invented. The regular replacement of fluids via intravenous injection was not a common practice. The use of personal protective equipment by doctors, nurses and aides was rudimentary, at best.
Another factor that compounded the challenges within the health-care system was a shortage of experienced medical staff.
When the Spanish flu emerged, the First World War was still raging across Europe. More than half of Canada’s physicians and thousands of nurses served overseas, the Canadian War Museum says.
Health care also wasn’t available to everyone in Winnipeg in 1918. Universal health care would not appear for decades.
As well, hospitals were often crowded and poorly ventilated.
“All of that has made it difficult for us to compare back to 100 years ago, because of how quickly health infrastructure and technology have increased,” Kindrachuk said.
“That being said, with all that, we still are at a point where there’s a million people that are dead [worldwide],” he said.
“That is what suggests to me that, yes, the numbers paint one picture of 1918, but certainly we have to be appreciative of all these variables that we actually have at our disposal and we’re still facing a difficult situation.”
Correction: CBC News originally reported that cases of the Spanish flu eventually disappeared from Winnipeg in the summer of 2019. It was the summer of 1919 when new cases were no longer found in Winnipeg.

Devoted web advocate. Bacon scholar. Internet lover. Passionate twitteraholic. Unable to type with boxing gloves on. Lifelong beer fanatic.





